At present, the health care workers working in the hospitals are facing the risk of transmission of COVID-19 world-wide; among which nurses are at higher risk. The infectious disease outbreaks in India have witnessed loss of life of nurse whether it was the NIPAH virus outbreak in Kerala during 2018 or the current pandemic of COVID-19. We have been hearing the nurses infected with COVID-19 since the time COVID-19 surge was seen in the country; with Delhi being the first state to report COVID-19 infection in a nurse. Since then, many nurses have been infected with COVID-19 across the country.

Higher risk of COVID-19 among nurses is related to multiple reasons
Our health care system is structured in such a way that the nurses are available beside patient for 24*7 to provide nursing care with the minimum distance from the patient for the range of services starting from administering medication to promoting personal hygiene of patient such as oral care, hair care, bed bath etc. This, by default would increase the exposure of nurses to the invisible contagious virus through the respiratory droplets.
The hazardous exposure of virus among nurses has also been a result of lack of Personal Protective Equipments (PPEs) or supply of poor quality PPEs. During this pandemic many hospitals ran out of PPE kits. There were instances where the nurses had been told to re-use disposable PPEs.1
A nurse has been threatened for refusing throat swab collection from a suspected case of COVID-19 because of lack of proper training and guidance. She was forced to collect the throat swab.2 Taking the throat swab like every time she does is not advisable when the virus is known to be highly contagious. This will put herself in a greater risk.
A recent newspaper clipping reported that the nurses were provided inadequate institutional quarantine support; after 14 days of shift in COVID-19 wards. They have been quarantined in the facility where nine people had to share a single bathroom.3 This was later brought into the attention of the government. However, in such situation, the risk of COVID-19 from each of them would be persistent even after returning from work. Few nurses returned to home quarantine due to lack of basic facilities at the quarantine centre by risking their immediate family members as well. Lack transportation facility for nurses to go for work during lockdown made them walk to reach the hospital increasing the likelihoods of spreading the infection to the people on the street and causing physical distress to nurses at work.4 The risk will always be there, but few safety measures can minimise the risk and promote safety of nurses.
Promotion of safety measures to minimise the risk of transmission irrespective of patient’s disease condition
v
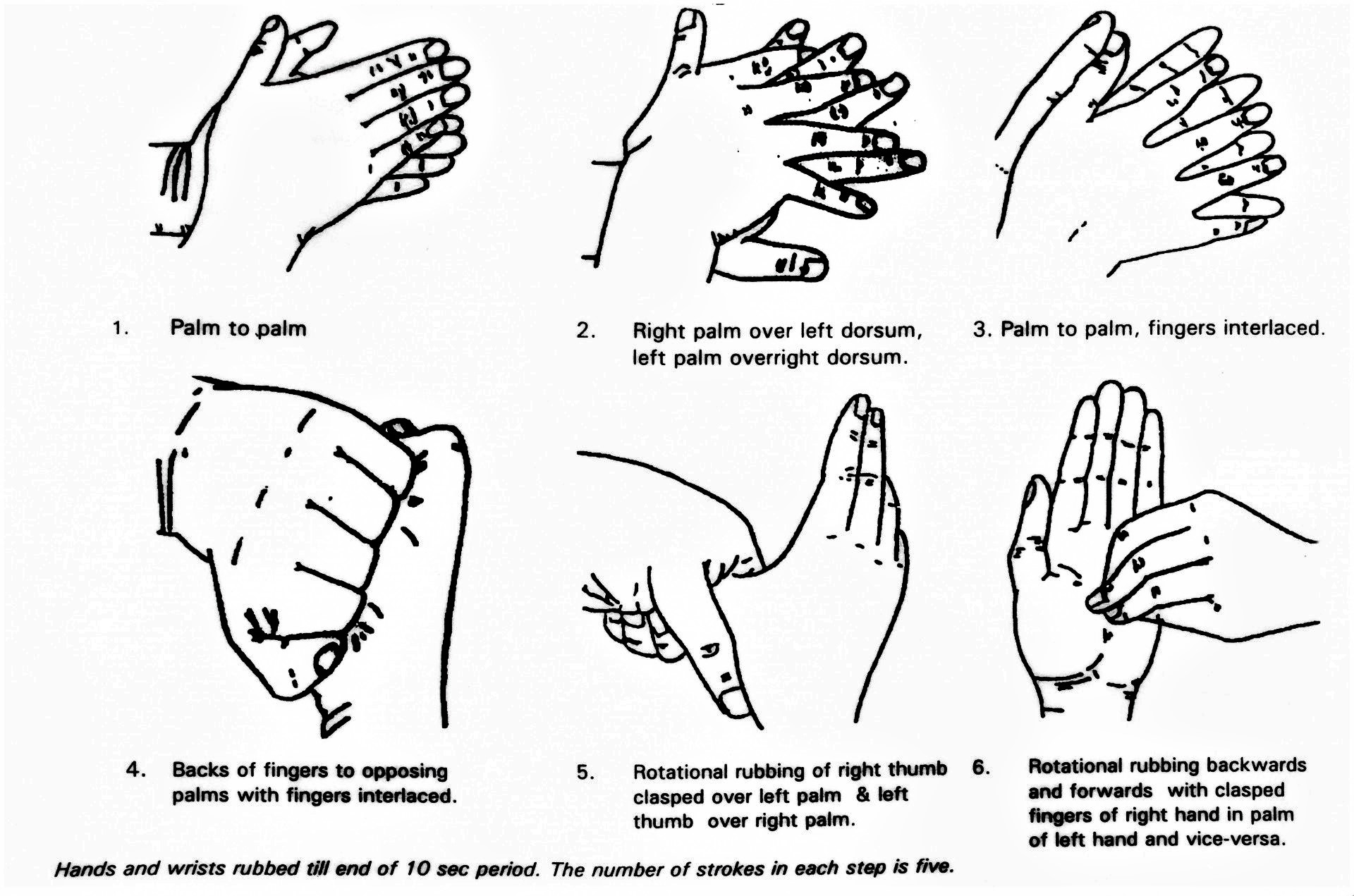
Provide adequate PPEs, sanitizer, disinfectants and proper disposal of PPEs is important to practice. Hand hygiene is key. Follow the WHO guidelines of hand hygiene.
v
Provide adequate education and training to nurses at different units with the recent guidelines of Ministry of Health and Family Welfare. Promote “No contact communication” with other health care professionals and hospital staffs wherever possible.
v
Schedule the nurses’ shift duties such that minimum exposure (avoid extra staffs, keep optimal staffs on duty) and common exposure (same staffs will continue to work at common shift for a defined period of time) is promoted.
v
Eat a healthy diet rich in Vitamin C and keep hydrated and exercise to remain physically and mentally fit.
v
Support each other psychologically to remain strong and calm. Providing counselling to the nurses working in isolation in order to relieve mental stress.
v
Providing transportation facility to the nurses to travel to workplace in order to reduce the risk of spreading the infection to other people and minimizing the physical distress among nurses at work.
v
Nurses with co-morbidities such as cardiovascular diseases, Diabetes, respiratory illness and immunosuppressed staffs should not be allowed to work in COVID-19 wards, emergency or critical care units until this pandemic comes to an end.
v
Pregnant and lactating mothers, and mothers of under-five children should be supported and make sure they do not expose to high risk units within hospital.

While combating this pandemic there are many factors affecting the physical and mental health of the nurses. The precautionary measures by wearing the PPE would limit intake of food, water and use of washrooms during duty hours. In addition to that continuous wearing a PPE does not allow air to pass through the body is will worsen the situation. The fear of contracting the disease, fear of endangering the lives of family members, fear of death, anxiety, stress and lack social support would aggravate the situation. This pandemic may come to an end. But the physical and psychological trauma may exist. Therefore, it becomes vital to support nurses in all the ways possible.
The issues mentioned in the blog has been referred to the following newspaper clippings-
https://indianexpress.com/article/cities/delhi/nurses-death-colleagues-say-had-to-wear-used-ppes-6427321/
https://www.indiatoday.in/india/story/forced-to-collect-samples-for-covid-19-testing-without-proper-training-nurses-complain-at-bengal-govt-hospital-1672934-2020-04-30
Photographs are taken from Google with the user rights
Written by Sushma Marita D’souza (BSc Nursing, MPH) and Pashanthi Kamath (BSc Nursing, MPH)






Great read! I really appreciate you for generating awareness among the workforce in this crucial time.
Excellent article mam!! Keep writing more! It’s really good to see in your article mentioning to refer guidelines from who and mohfw is appreciable and it really helps to fight the fake news and information..